Effective antimicrobial stewardship interventions need to improve patient outcomes to be deemed successful. The ASP team at Eastern Health recently published a study proving the impact of using the Firstline app to dramatically improve patient outcomes at their hospital. Key findings showed a +10.5% increase in prescribing appropriateness, along with a dramatic savings of $550/bed/year, through reductions in antimicrobial use and C. difficile infections.
We recently interviewed the ASP leads at Eastern Health, Dr. Peter Daley and Gerry McDonald, BSc. Pharm, about this exciting study to gain their insights on the findings. Dr. Peter Daley (PD) is the co-chair of the provincial AMS Committee in Newfoundland, Canada. Gerry McDonald, BSc. Pharm (GM), is a full-time Antimicrobial Stewardship Pharmacist with Eastern Health and co-chair of the regional Antimicrobial Stewardship Committee.
What made you interested in studying the impact of a mobile app on your stewardship outcomes?
PD: It’s important that stewardship interventions are evidence-based. Like infection control interventions, stewardship interventions are often studied in time series designs, like ours, but they should ideally be subjected to randomized or cluster randomized trials. Furthermore, outcomes of stewardship should be more than just reduction in antimicrobial use, but include qualitative prescribing (appropriateness) and patient-centered outcomes such as C.difficile rate, length of stay, readmission and mortality.
GM: When we conceptualized and proposed the Firstline implementation at Eastern Health, we were quite confident it would be well received and used, but in today’s healthcare environment, you need to prove what you are doing provides value to achieve sustainability. Not only did this study contribute to the body of knowledge surrounding mobile device applications in antimicrobial stewardship, but it also financially justified continuing with this product in our health region.
What obstacles did you face in implementing the study and how did you overcome them?
PD: Our health region needed to be convinced to pay the fee for the Firstline subscription. We started on a trial and demonstrated the financial impact to justify funding.
GM: We had some data collection challenges at the outset which were a bit more challenging than I anticipated (particularly in obtaining Antimicrobial use data). Happy to say while some challenges still exist there, we have become much more sophisticated in our analysis now and this process continues as an ongoing quality control measure.
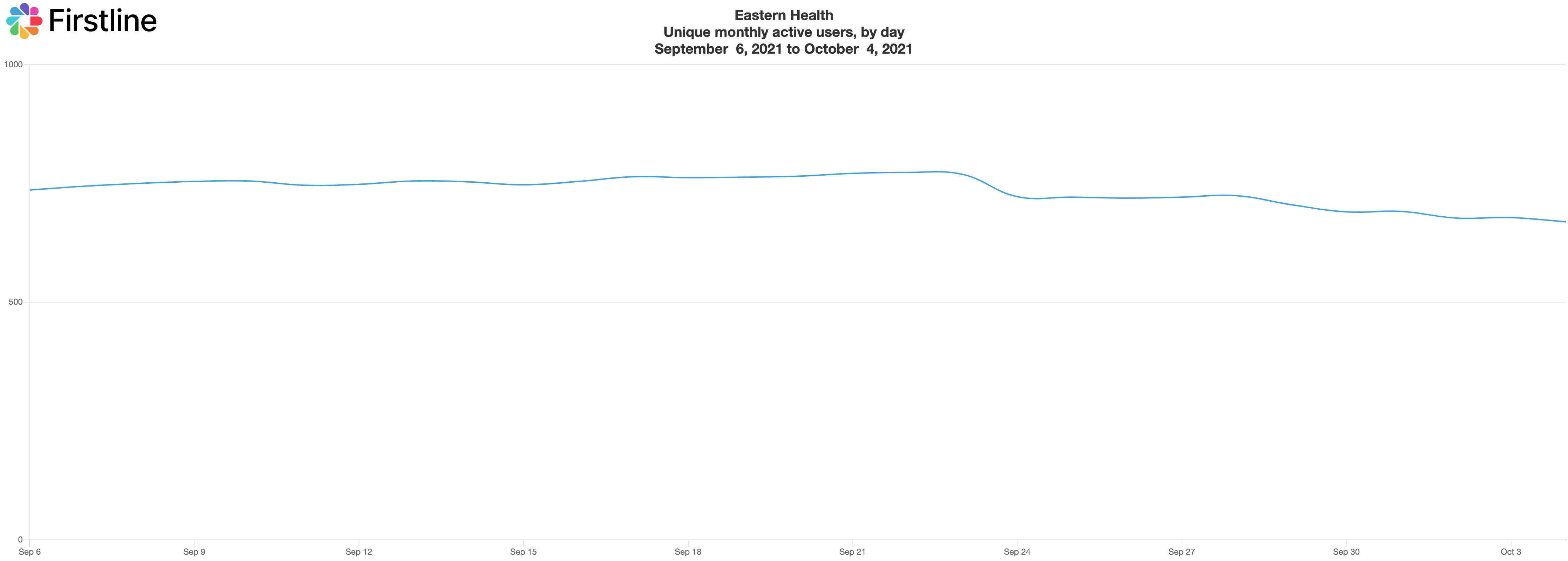
You have 690 active users regularly using the Firstline app. How was the app first received by providers? How did you get so many people to use it? What kinds of feedback did you hear when you first implemented it?
PD: We positioned the app as offering province-specific recommendations based on a low rate of antimicrobial resistance compared to other settings, making it distinct from competitor resources. We used the app to teach medical students and residents. We encourage our infectious diseases telephone consultations to use the app. Feedback has been positive from physicians and administrators.
GM: Many of my colleagues were already familiar with Firstline prior to us adopting it and were absolutely ecstatic to find out we were adding our own local treatment recommendations and resistance data. Many were using competitor’s products which contained recommendations based on resistance patterns that were not applicable to our region and some drugs that were not even available in Canada. The customization that Firstline allowed us to make proved to be a much better fit and facilitated uptake among various groups.
One of the main outcomes of the study were significant reductions in AMU and in CDI. You saved more than $550 per bed per year as the result of implementing Firstline. How did this align with your expectations?
PD: We know that antimicrobial stewardship interventions save money and reduce AMU, but we needed to measure this. We think that they reduce AMR as well, but there are more variables involved in AMR than only AMU. We know that physicians overtreat, and that patients do well with less duration and narrower spectrum of activity, leading to earlier discharge.
GM: I think there will always be a few people who will resist changes in practice no matter what is presented to them, but there are also many who are just looking for the best information they can find in a readily accessible format to inform decision making. I think the outcomes were a great initial step in improving prescribing patterns but need to be augmented with other stewardship/IPAC interventions to keep things moving in the right direction.
Now that the study has been published and the outcomes were so impressive, what reaction have you seen from providers? From hospital administration? From colleagues?
PD: Administrators have been happy with the results, but unfortunately we have not yet translated this into support for AMS staffing. AMS is still a low priority to administration despite accreditation requirements.
GM: Feedback from administration has been positive, and I have had people say to me personally that it’s good to see all the hard work that went into this from our Stewardship committee as a whole lead to beneficial outcomes. There are probably many users who aren’t familiar with the study results but as long as they continue to use the app and encourage their colleagues to do so, I’ll take it!
What do you think it is about Firstline’s platform that created such an impact in your stewardship program?
PD: The recommendations in Firstline are based on our local AMR rates. Prescribers are also using UptoDate, Sanford, Bugs and Drugs.
GM: The fact that Firstline is highly customizable to our drug formulary (inpatient and outpatient) – and easy to make the edits from the administrator platform has made a big impact for us. Also Firstline’s Community Resource Library allowed us to adapt content from other Health Authorities without having to compose every word from scratch – made a HUGE difference in preparing content prior to launch.
View Eastern Health’s guidelines
What would you tell another ASP who is considering using a mobile app to improve their stewardship program?
GM: I definitely recommend it. It’s a bit of work getting it set up, but once implemented it’s a cost effective and convenient means of disseminating guidelines and therapy recommendations. (Of course, as with any educational intervention, impact will be limited without other complementary stewardship interventions).
Given the results you saw from the study, how will this inform your ASP plans going forward?
PD: We will continue to use the Firstline app, among other interventions such as audit and feedback. Our focus is outpatient antimicrobial initiation for mild respiratory tract infections, so we are surveying patterns from our pharmacy network. We would like to use point of care biomarkers in primary care.
GM: We anticipate this will continue to be a big part of both regional and provincial stewardship efforts going forward, and hope to continue to expand/customize content.
Where do you think the next improvements in prescribing appropriateness at your ASP will come from?
PD: Hopefully in primary care, where most antibiotics are used.
GM: I am also a member of the Provincial Stewardship Committee, so even though I practice in an acute care inpatient setting, I always think of the outpatient world when I think of opportunities to optimize antimicrobial prescribing practice. The majority of antimicrobials are used by outpatients, and despite some improvements Newfoundland continues to have rather high outpatient AMU rates. Improved stewardship in this area, particularly respiratory and urinary tract infections, would benefit everyone moving forward.
Join Peter Daley and Gerry McDonald and other ASP leads in the new Firstline Community - a free platform connecting all infectious disease specialists, to share guidelines, learn from each other and spread trusted knowledge.